The heart is the engine inside your body that keeps everything operational. In principle, the heart is a muscular pump that maintains oxygen and blood circulation through your lungs and body. In a day, your heart pumps about 2,000 gallons of blood. Like any engine, if the heart is not well taken care of it can break down and pump less efficiently, a condition called heart failure.
Until recently, the only solution for many severe heart failure patients has been heart transplants. However, there are only slightly more than 5,000 heart transplants performed in the world in a year, meaning that tens of thousands of people die waiting for a donor heart. On July 2, 2001, heart failure patients were given new hope as surgeons at Jewish Hospital in Louisville, Kentucky, performed the first artificial heart transplant in nearly two decades. The AbioCor Implantable Replacement Heart is the first completely self-contained artificial heart and is expected to at least double the life expectancy of heart patients.
In this article, you will acquire an in-depth understanding on how this new artificial heart works, how it's implanted into a patient's chest and who might be a candidate for receiving one of these mechanical hearts. We will also compare the AbioCor heart to the artificial hearts that have proved failure in the past.
Until recently, the only solution for many severe heart failure patients has been heart transplants. However, there are only slightly more than 5,000 heart transplants performed in the world in a year, meaning that tens of thousands of people die waiting for a donor heart. On July 2, 2001, heart failure patients were given new hope as surgeons at Jewish Hospital in Louisville, Kentucky, performed the first artificial heart transplant in nearly two decades. The AbioCor Implantable Replacement Heart is the first completely self-contained artificial heart and is expected to at least double the life expectancy of heart patients.
In this article, you will acquire an in-depth understanding on how this new artificial heart works, how it's implanted into a patient's chest and who might be a candidate for receiving one of these mechanical hearts. We will also compare the AbioCor heart to the artificial hearts that have proved failure in the past.
A Hydraulic-driven Heart
The average adult human heart pumps blood at a rate of 60 to 100 times per minute. If you've read how your heart works, then you know that the heart contracts in two stages:
Patients with an implanted AbioCor heart will still have atria that beat at the same time, but the artificial heart, which replaces both ventricles, can only force blood out one ventricle at a time. So, it will alternately send blood to the lungs and then to the body, instead of both at the same time as a natural heart does. The AbioCor is able to pump more than 10 liters per minute, which is enough for everyday activities.
The average adult human heart pumps blood at a rate of 60 to 100 times per minute. If you've read how your heart works, then you know that the heart contracts in two stages:
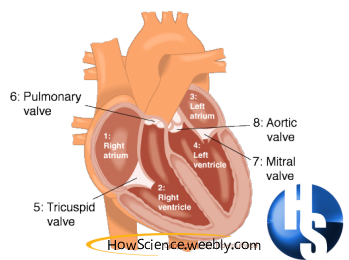
- In the first stage, the right and left atria contract at the same time, pumping blood to the right and left ventricles.
- In the second stage, the ventricles contract together to propel blood out of the heart.
Patients with an implanted AbioCor heart will still have atria that beat at the same time, but the artificial heart, which replaces both ventricles, can only force blood out one ventricle at a time. So, it will alternately send blood to the lungs and then to the body, instead of both at the same time as a natural heart does. The AbioCor is able to pump more than 10 liters per minute, which is enough for everyday activities.
The AbioCor, developed by Abiomed, is a very sophisticated medical device, but the core mechanism of the device is the hydraulic pump that shuttles hydraulic fluid from side to side. To understand how it works, let's look at the various components of the system:
- Hydraulic pump - The basic idea with this device is similar to the hydraulic pumps used in heavy equipments. Force that is applied at one point is transmitted to another point using an incompressible fluid. A gear inside the pump spins at 10,000 revolutions per minute (rpm) to create pressure.
- Porting valve - This valve opens and closes to let the hydraulic fluid flow from one side of the artificial heart to the other. When the fluid moves to the right, blood gets pumped to the lungs through an artificial ventricle. When the fluid moves to the left, blood gets pumped to the rest of the body.
- Wireless energy-transfer system - Also called the Transcutaneous Energy Transfer (TET), this system consists of two coils, one internal and one external, that transmit power via magnetic force from an external battery across the skin without piercing the surface. The internal coil receives the power and sends it to the internal battery and controller device.
- Internal battery - A rechargeable battery is implanted inside the patient's abdomen. This gives a patient 30 to 40 minutes to perform certain activities, such as showering, while disconnected from the main battery pack.
- External battery - This battery is worn on a Velcro-belt pack around the patient's waist. Each rechargeable battery offers about four to five hours of power.
- Controller - This small electronic device is implanted in the patient's abdominal wall. It monitors and controls the pumping speed of the heart.
- Right atrium
- Left atrium
- Aorta
- Pulmonary artery
The Seven-hour Surgery
The surgery to implant an AbioCor artificial heart is extremely delicate. Not only are the surgeons cutting off and extracting the natural heart's right and left ventricles, but they are also placing a foreign object into the patient's chest. The patient must be placed on, and later removed from, a heart-lung machine. The surgery requires hundreds of stitches, to properly secure the heart to artificial ventricles. Grafts connect the AbioCor to remaining parts of the natural heart. Grafts are a kind of synthetic tissue used to connect the artificial device to the patient's natural tissue.
Due to the complexity of the surgery, there are lots of medical personnel on-hand during the operation. The surgery on July 2, 2001, which was the first of its kind in the world, included a team of the two lead surgeons, 14 nurses, perfusionists, anesthesiologists and other support staff.
Here is the procedure, as described by University of Louisville surgeon Robert Dowling:
Originally, Abiomed officials cautioned against overly-optimistic results; the most optimistic predictions were that a patient could live up to six months with the AbioCor heart. The device is only designed to double life expectancy for patients who had only about 30 days to live prior to the operation.
Robert Tools, the patient who received the heart transplant on July 2, 2001, at Jewish Hospital in Louisville, has passed away. Ten other patients have also died, but the recipients of the AbioCor heart have lived an average of five months after their transplants.
The surgery to implant an AbioCor artificial heart is extremely delicate. Not only are the surgeons cutting off and extracting the natural heart's right and left ventricles, but they are also placing a foreign object into the patient's chest. The patient must be placed on, and later removed from, a heart-lung machine. The surgery requires hundreds of stitches, to properly secure the heart to artificial ventricles. Grafts connect the AbioCor to remaining parts of the natural heart. Grafts are a kind of synthetic tissue used to connect the artificial device to the patient's natural tissue.
Due to the complexity of the surgery, there are lots of medical personnel on-hand during the operation. The surgery on July 2, 2001, which was the first of its kind in the world, included a team of the two lead surgeons, 14 nurses, perfusionists, anesthesiologists and other support staff.
Here is the procedure, as described by University of Louisville surgeon Robert Dowling:
- Surgeons implant the energy-transfer coil in the abdomen.
- The breast bone is opened and the patient is placed on a heart-lung machine.
- Surgeons remove the right and left ventricles of the native heart. They leave in the right and left atria, the aorta and the pulmonary artery. This part of the surgery alone takes two to three hours.
- Atrial cuffs are sewn to the native heart's right and left atria.
- A plastic model is placed in the chest to determine the proper placement and fit of the heart in the patient.
- Grafts are cut to an appropriate length and sewn to the aorta and pulmonary artery.
- The AbioCor is placed in the chest. Surgeons use "quick connects" -- sort of like little snaps -- to connect the heart to the pulmonary artery, aorta and left and right atria.
- All of the air in the device is removed.
- The patient is taken off the heart-lung machine.
- The surgical team ensures that the heart is working properly.
Originally, Abiomed officials cautioned against overly-optimistic results; the most optimistic predictions were that a patient could live up to six months with the AbioCor heart. The device is only designed to double life expectancy for patients who had only about 30 days to live prior to the operation.
Robert Tools, the patient who received the heart transplant on July 2, 2001, at Jewish Hospital in Louisville, has passed away. Ten other patients have also died, but the recipients of the AbioCor heart have lived an average of five months after their transplants.
The Jarvik-7
In 1982, Dr. William Devries implanted the Jarvik-7, the first device designed to be a completely permanent replacement heart. The surgery was done at the University of Utah, and the patient was Dr. Barney Clark, a dentist from Seattle. Clark lived for 112 days on the heart before succumbing to complications caused by the device.
The Jarvik-7 was an air-driven heart designed by Dr. Willem Kolff and Dr. Don Olsen. Unlike the self-contained AbioCor, the Jarvik-7 heart required several external wires, which protruded from the patient and connected to a large external unit. These protruding wires led to several infections in Clark.
Four more patients received the Jarvik-7 before it was discontinued due to complications, including stroke, mechanical failure and anatomical fit issues. It has since been enhanced and renamed, now called the CardioWest heart. It is used only in experimental situations and as an investigative bridge-to-transplantation device.
In 1982, Dr. William Devries implanted the Jarvik-7, the first device designed to be a completely permanent replacement heart. The surgery was done at the University of Utah, and the patient was Dr. Barney Clark, a dentist from Seattle. Clark lived for 112 days on the heart before succumbing to complications caused by the device.
The Jarvik-7 was an air-driven heart designed by Dr. Willem Kolff and Dr. Don Olsen. Unlike the self-contained AbioCor, the Jarvik-7 heart required several external wires, which protruded from the patient and connected to a large external unit. These protruding wires led to several infections in Clark.
Four more patients received the Jarvik-7 before it was discontinued due to complications, including stroke, mechanical failure and anatomical fit issues. It has since been enhanced and renamed, now called the CardioWest heart. It is used only in experimental situations and as an investigative bridge-to-transplantation device.




 RSS Feed
RSS Feed
